Scientific Advisor : Elmira Narmatova, Associate Professor,IMF-OSHSU
Authored By : Ahmed Shakeel , Almas Arif ; 3rd Year MBBS,IMF-OSHSU
Subject: Pediatrics (Child Diseases)
International Medical Faculty
Osh State University
Year: 2026
Abstract
Iron deficiency anemia (IDA) is the most common nutritional disorder affecting children worldwide and remains a major public health challenge, particularly in low- and middle-income countries. Childhood IDA is associated with impaired cognitive development, reduced immunity, poor growth, and increased morbidity and mortality. This article reviews iron deficiency anemia in children using evidence derived from two large population-based surveys conducted in different geographical and socio-economic contexts: the National Family Health Survey-5 (NFHS-5) from India (2019–2021) and the National Integrated Micronutrient and Anthropometric Survey (NIMAS) from the Kyrgyz Republic (2021). The methodology, prevalence, and key determinants of anemia among children are analyzed, and findings from both surveys are compared. The results highlight a persistently high burden of anemia among Indian children and a moderate but significant burden in Kyrgyzstan. Differences in dietary patterns, health systems, and public health interventions explain variations in prevalence. The article concludes with evidence-based recommendations for prevention, early detection, and control of iron deficiency anemia in children.
Keywords: Iron deficiency anemia, children, NFHS-5, NIMAS, micronutrient deficiency
Iron deficiency anemia (IDA) is defined as a condition in which hemoglobin levels fall below normal due to insufficient iron availability for hemoglobin synthesis. Iron is essential for oxygen transport, cellular respiration, neurological development, and immune function. Children are particularly vulnerable to iron deficiency because of rapid growth, increased iron requirements, and often inadequate dietary intake [1].
Globally, anemia affects approximately 40% of children aged 6–59 months, making it a leading contributor to childhood morbidity [2]. Although anemia has multiple causes, iron deficiency accounts for nearly half of all anemia cases in children worldwide [3]. The consequences of IDA in childhood include delayed psychomotor development, poor school performance, behavioral problems, and increased susceptibility to infections [4].
South Asia has one of the highest burdens of childhood anemia globally, with India contributing a substantial proportion of cases [5]. In contrast, Central Asian countries such as the Kyrgyz Republic have lower prevalence but still face significant micronutrient deficiencies due to dietary inadequacies and socio-economic transitions [6].
Large-scale population-based surveys are essential for understanding the magnitude and determinants of anemia. This article focuses on two such surveys:
● NFHS-5 (India, 2019–2021)
● NIMAS (Kyrgyz Republic, 2021)
These surveys provide reliable, standardized data on anemia prevalence among children and allow meaningful cross-country comparison.
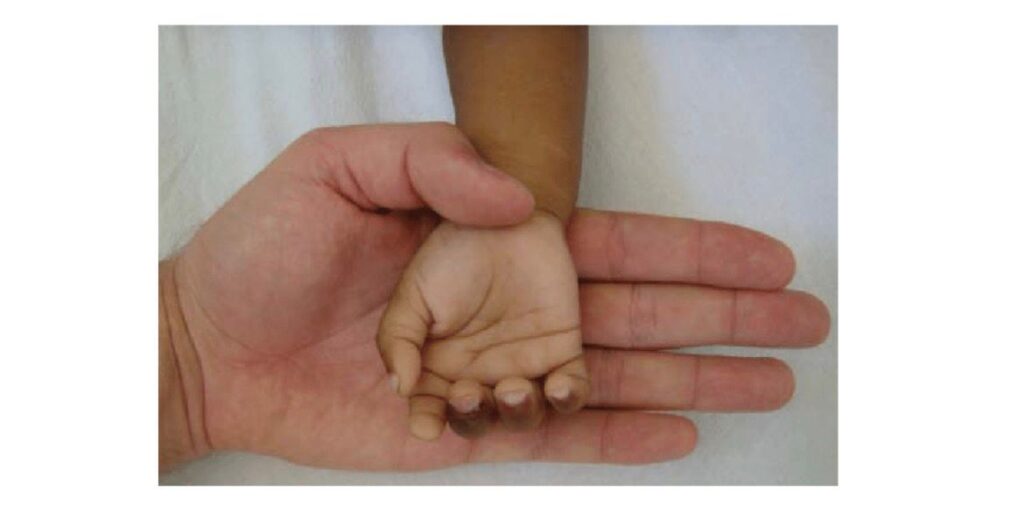
Table: a child having severe anemia
This article is a descriptive and comparative review based on secondary analysis of data from two nationally representative surveys:
1. National Family Health Survey-5 (NFHS-5), India
2. National Integrated Micronutrient and Anthropometric Survey (NIMAS), Kyrgyz Republic
In addition, peer-reviewed literature and global guidelines were reviewed to contextualize survey findings.
NFHS-5 is a large-scale, multi-round survey conducted under the Ministry of Health and Family Welfare, Government of India. It uses a stratified two-stage sampling design and covers all states and union territories. Hemoglobin estimation was done using capillary blood samples analyzed by portable HemoCue analyzers [7]. Children aged 6–59 months were classified as anemic based on WHO hemoglobin cut-offs (<11 g/dL).
The NIMAS survey was conducted nationally to assess micronutrient deficiencies among children and women. A multistage cluster sampling method was used. Venous blood samples were collected, and hemoglobin levels were measured using standardized laboratory methods. Iron deficiency was assessed using serum ferritin with adjustment for inflammation [8].
From both surveys, the following information was extracted:
● Sample size and age groups
● Methods of hemoglobin estimation
● Prevalence of anemia
● Key associated factors
No estimation or extrapolation was performed where data were not reported.
Burden of Anemia among Children in India (NFHS-5)
The National Family Health Survey-5 (2019–2021) demonstrates that anemia remains a severe public health problem among children aged 6–59 months in India. According to WHO classification, a prevalence above 40% constitutes a severe public health concern; India’s prevalence of childhood anemia far exceeds this threshold [7,10]. The survey reports that 67.1% of children aged 6–59 months are anemic, indicating that more than two out of every three children are affected [7].
Anemia prevalence shows marked rural–urban differentials, with higher prevalence observed in rural areas compared to urban areas. This disparity reflects differences in dietary diversity, access to health services, maternal education, and socio-economic conditions. NFHS-5 also reports minimal gender differences, suggesting that both male and female children are equally vulnerable during early childhood [7].
Younger children, particularly those aged 6–23 months, exhibit the highest anemia prevalence, corresponding to the period of rapid growth and transition from exclusive breastfeeding to complementary feeding. Inadequate iron intake during this critical window substantially increases the risk of iron deficiency anemia. Although NFHS-5 does not assess biochemical iron status, the high prevalence strongly suggests iron deficiency as a major contributor, consistent with global evidence [1,3].
Table 1: Prevalence of Anemia among Children (6–59 months) in India – NFHS-5
| Indicator | Prevalence (%) |
| Overall anemia prevalence | 67.1 |
| Urban children | 64.2 |
| Rural children | 69.4 |
| Male children | 66.4 |
| Female children | 67.8 |
Source: National Family Health Survey-5, India [7]
Burden of Anemia and Iron Deficiency among Children in the Kyrgyz Republic (NIMAS 2021)
The National Integrated Micronutrient and Anthropometric Survey (2021) provides comprehensive data on anemia and iron deficiency among children aged 6–59 months in the Kyrgyz Republic. The overall prevalence of anemia reported by NIMAS is 33.4%, which is classified as a moderate public health problem according to WHO criteria [8,10].
A major strength of the NIMAS survey is the inclusion of biochemical indicators of iron status, allowing differentiation between anemia and iron deficiency anemia. The survey reports that 42.1% of children have iron deficiency, while 21.3% suffer from iron deficiency anemia, confirming iron deficiency as the principal underlying cause of anemia in this population [8].
The findings indicate that a significant proportion of children with normal hemoglobin levels still have depleted iron stores, placing them at risk of developing anemia if preventive measures are not implemented. Dietary patterns characterized by limited intake of iron-rich and fortified foods were identified as important contributors. These findings underscore the importance of early prevention strategies rather than reliance on anemia treatment alone [8].
Table 2: Anemia and Iron Status among Children (6–59 months) in the Kyrgyz Republic – NIMAS 2021
| Indicator | Prevalence (%) |
| Anemia (Hb <11 g/dL) | 33.4 |
| Iron deficiency | 42.1 |
| Iron deficiency anemia | 21.3 |
Source: National Integrated Micronutrient and Anthropometric Survey, Kyrgyz Republic [8]
Comparative Analysis of Childhood Anemia: India and Kyrgyz Republic
A comparison of results from NFHS-5 and NIMAS reveals substantial differences in the magnitude of childhood anemia between the two countries. India demonstrates a very high prevalence, more than double that observed in the Kyrgyz Republic. However, both countries share iron deficiency as a dominant nutritional concern in early childhood [7,8].
The absence of biochemical iron markers in NFHS-5 limits precise attribution of anemia causes in India. In contrast, NIMAS provides a more nuanced understanding of iron deficiency and iron deficiency anemia through laboratory assessment. These methodological differences should be considered when interpreting cross-country comparisons [8,10].
Despite these differences, the findings from both surveys consistently highlight early childhood as a critical period for intervention. The results support WHO and UNICEF recommendations emphasizing prevention, dietary diversification, supplementation, and food fortification as essential strategies to reduce childhood anemia [1,2].
Table 3: Comparison of Childhood Anemia Indicators between India and Kyrgyz Republic
| Indicator | India (NFHS-5) | Kyrgyz Republic (NIMAS) |
| Survey year | 2019–2021 | 2021 |
| Age group | 6–59 months | 6–59 months |
| Anemia prevalence (%) | 67.1 | 33.4 |
| Iron deficiency assessed | Not reported | Yes |
| Iron deficiency anemia (%) | Not reported | 21.3 |
Sources: NFHS-5 [7]; NIMAS 2021 [8]
Overall, the results indicate that childhood anemia remains widespread and severe in India, while Kyrgyzstan experiences a moderate but significant burden of anemia and iron deficiency. The data emphasize the importance of improving dietary iron intake, strengthening supplementation and fortification programs, and enhancing anemia surveillance systems. These findings align closely with global evidence and reinforce the need for sustained, evidence-based public health interventions [1,2,3].
The findings demonstrate a stark contrast between India and the Kyrgyz Republic in terms of childhood anemia burden. India shows an alarmingly high prevalence, reflecting persistent nutritional challenges despite long-standing national programs such as the Iron and Folic Acid (IFA) supplementation and food fortification initiatives [9].
In contrast, Kyrgyzstan exhibits a lower prevalence, possibly due to better maternal literacy, smaller population size, and more uniform access to healthcare. However, the high prevalence of iron deficiency suggests potential future increases in anemia if preventive strategies are not strengthened [8].
Methodological differences, such as the use of capillary versus venous blood samples and lack of ferritin measurement in NFHS-5, may partly explain variations between surveys [10]. Nonetheless, both surveys underscore iron deficiency as a critical public health issue.
Conclusion and Recommendations
Iron deficiency anemia remains a major public health problem among children and continues to pose a significant threat to child survival, growth, and development. Evidence from nationally representative surveys conducted in India and the Kyrgyz Republic demonstrates that anemia affects a substantial proportion of children under five years of age, with iron deficiency being a predominant underlying cause. Despite differences in prevalence between countries, childhood anemia persists across diverse settings, indicating the need for sustained and context-specific interventions.
The findings from the National Family Health Survey-5 indicate that anemia among Indian children remains at an unacceptably high level, reflecting persistent nutritional inadequacies and ongoing exposure to preventable risk factors. Similarly, results from the National Integrated Micronutrient and Anthropometric Survey in the Kyrgyz Republic reveal a considerable burden of iron deficiency and iron deficiency anemia, highlighting that micronutrient deficiencies remain a concern even in settings with comparatively lower anemia prevalence. These findings are consistent with global estimates reported by the World Health Organization and UNICEF, which identify anemia as one of the most widespread nutritional disorders in childhood.
Childhood iron deficiency anemia has well-documented adverse consequences, including impaired cognitive and motor development, weakened immune function, reduced physical capacity, and increased risk of morbidity. When anemia occurs during critical periods of growth and brain development, its effects may be long-lasting and may contribute to poor educational outcomes and reduced economic productivity in adulthood. Therefore, prevention and control of iron deficiency anemia in children is not only a health priority but also a key investment in human capital development.
The survey findings further emphasize the importance of strengthening national anemia surveillance systems. Reliance on hemoglobin concentration alone limits the ability to accurately identify iron deficiency anemia, particularly in populations where infections and inflammation are common. The inclusion of additional biomarkers of iron status, such as serum ferritin with appropriate adjustment for inflammation, is essential for guiding effective public health responses.
In line with WHO and UNICEF guidance, the following evidence-based recommendations are proposed:
1. Strengthen Prevention Across the Life Course
Prevention of childhood anemia should begin before birth through improved maternal nutrition, adequate antenatal care, and prevention of maternal anemia. Interventions should continue throughout infancy and early childhood, particularly during the first 1,000 days of life.
2. Promote Optimal Infant and Young Child Feeding Practices
Appropriate complementary feeding practices should be promoted, with emphasis on timely introduction of nutritionally adequate, diverse, and iron-rich foods. Caregivers should be supported through nutrition education and behavior change communication to improve dietary quality and iron bioavailability.
3. Ensure Effective Micronutrient Supplementation
Iron supplementation programs should be implemented in accordance with national and WHO recommendations, with particular focus on high-risk populations. Program effectiveness should be enhanced through regular monitoring, quality assurance, and strategies to improve adherence.
4. Expand and Monitor Food Fortification
Fortification of commonly consumed staple foods with iron should be strengthened as a population-wide strategy to reduce iron deficiency. Fortification programs must be supported by regulatory oversight and continuous monitoring to ensure safety and effectiveness.
5. Address Infection and Inflammation-Related Causes of Anemia
Integrated approaches including deworming, malaria control where applicable, immunization, and improvements in water, sanitation, and hygiene are essential components of anemia reduction strategies.
6. Improve Data Quality and Surveillance
Future national surveys should incorporate comprehensive assessment of iron status, including biochemical indicators beyond hemoglobin. High-quality data are critical for monitoring progress toward global nutrition targets and for guiding policy decisions.
7. Adopt a Multisectoral Approach
Reduction of childhood anemia requires coordinated action across health, nutrition, education, agriculture, and social protection sectors. Strong political commitment, sustained financing, and community engagement are essential for achieving meaningful and lasting reductions in anemia prevalence.
In conclusion, iron deficiency anemia in children remains a preventable condition with significant implications for child health and development. The evidence from India and the Kyrgyz Republic underscores the urgent need to scale up comprehensive, evidence-based interventions aligned with global recommendations. Accelerated action is required to achieve national and global targets for anemia reduction and to ensure that all children attain their full growth and developmental potential.
1. World Health Organization.
Iron Deficiency Anaemia: Assessment, Prevention and Control. WHO, Geneva; 2001.
This guideline provides standardized definitions, diagnostic criteria, and public health strategies for iron deficiency anemia, especially in children and women. It remains a foundational reference for anemia control programs worldwide.
🔗https://www.who.int/publications/i/item/WHO-NHD-01.3
2. World Health Organization.
The Global Prevalence of Anaemia in 2011.WHO; 2015.
This report presents global and regional estimates of anemia prevalence using pooled population-based data. It highlights children under five as one of the most affected groups globally.
🔗https://apps.who.int/iris/handle/10665/177094
3. Kassebaum NJ, et al.
A systematic analysis of the global burden of anemia from 1990 to 2010. The Lancet. 2014.
This Global Burden of Disease study quantifies anemia prevalence and disability worldwide and identifies iron deficiency as the leading cause. It provides strong epidemiological evidence on anemia trends.
🔗https://www.sciencedirect.com/science/article/pii/S0140673613622784
4. Lozoff B, et al.
Long-lasting neural and behavioral effects of iron deficiency in infancy. Pediatrics. 2006.
This study demonstrates that iron deficiency in early life can lead to persistent cognitive and behavioral deficits. It emphasizes the importance of early prevention of childhood anemia.
🔗https://publications.aap.org/pediatrics/article/117/2/e494/69591
5. Stevens GA, et al.
Global trends in hemoglobin concentration and anemia prevalence. Am J Clin Nutr. 2013.
This paper analyzes anemia trends among children and women across regions, identifying South Asia as a high-burden area. It supports the continued public health relevance of anemia.
🔗https://academic.oup.com/ajcn/article/98/3/1/4577257
6. UNICEF.
Micronutrient Deficiencies in Central Asia.UNICEF; 2020.
This report reviews the burden of micronutrient deficiencies, including iron deficiency, in Central Asian countries. It provides regional context for childhood anemia in Kyrgyzstan.
🔗 https://www.unicef.org/eca/reports
7. Ministry of Health and Family Welfare, Government of India.
National Family Health Survey (NFHS-5), 2019–21. IIPS; 2021.
NFHS-5 provides nationally representative data on anemia among Indian children aged 6–59 months using hemoglobin estimation. It is the primary source for childhood anemia prevalence in India.
🔗 https://nfhsindia.org/nfhs-5
8. Ministry of Health, Kyrgyz Republic; UNICEF; WHO.
National Integrated Micronutrient and Anthropometric Survey (NIMAS), 2021.
This survey assesses anemia, iron deficiency, and iron deficiency anemia using biochemical markers in children. It provides high-quality national data for Kyrgyzstan.
🔗https://groundworkhealth.org/resources/nimas-2021-kyrgyz-republic/
9. Government of India.
National Iron Plus Initiative (NIPI) Guidelines.MoHFW; 2018.
These guidelines outline India’s life-cycle approach to iron and folic acid supplementation. They form the policy basis for anemia prevention programs in children.
🔗https://nhm.gov.in/images/pdf/programmes/child-health/guidelines/NIPI_Guidelines.pdf
10. World Health Organization.
Haemoglobin Concentrations for the Diagnosis of Anaemia. WHO; 2011.
This document defines hemoglobin cut-off values for diagnosing anemia across age groups. It is widely used in surveys and clinical practice.
🔗https://www.who.int/publications/i/item/WHO-NMH-NHD-MNM-11.1
11. Black RE, et al.
Maternal and child undernutrition in low- and middle-income countries. The Lancet. 2013.
This series links micronutrient deficiencies, including anemia, to child morbidity and mortality. It highlights anemia as a major contributor to poor child outcomes.
🔗 https://www.thelancet.com/series/maternal-and-child-nutrition
12. Pasricha SR, et al.
Iron deficiency. Blood. 2021.
This review explains iron metabolism, causes of iron deficiency, and diagnostic challenges. It provides updated scientific understanding relevant to pediatric anemia.
🔗https://ashpublications.org/blood/article/138/1/30/475302
13. UNICEF, WHO, World Bank.
Joint Child Malnutrition Estimates. 2020.
This report provides global data on child malnutrition and discusses the interaction between undernutrition and anemia. It supports integrated nutrition strategies.
🔗 https://www.who.int/teams/nutrition-and-food-safety/monitoring-nutrition/joint-child-malnutrition-estimates
14. Beard JL.
Iron biology in immune and neural function. Journal of Nutrition. 2001.
This article explains the role of iron in immunity, brain development, and muscle function. It supports the biological importance of preventing iron deficiency anemia.
🔗https://academic.oup.com/jn/article/131/2/568S/4687088
